THE PLEURA
Pleura is a serous membrane covered by mesothelium. There are two pleural sacs right and left covering respective lungs.
It shows two layers 1. Visceral or pulmonary 2. Parietal. These two layers are continuous with each other near hilum of lung. It forms a space between two layers known as pleural cavity.
1. Visceral or pulmonary pleura :
It covers surface of lung firmly attached to it. At hilum and pulmonary ligaments it continue as parietal pleura. It goes around the root of lung downwards as a fold of pulmonary ligament.
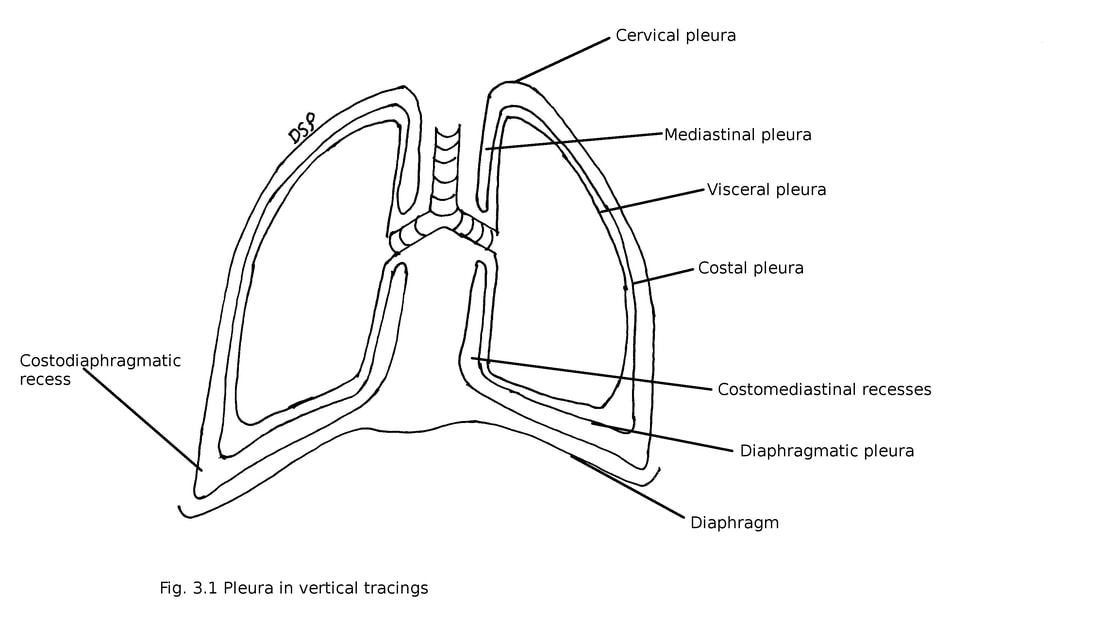
2. Parietal pleura : It shows attachment on inner surface of sternum, ribs, intercostal spaces, costal cartilages, diaphragm and vertebra. It shows four parts : 1) costal 2) diaphragmatic 3) cervical 4) mediastinal
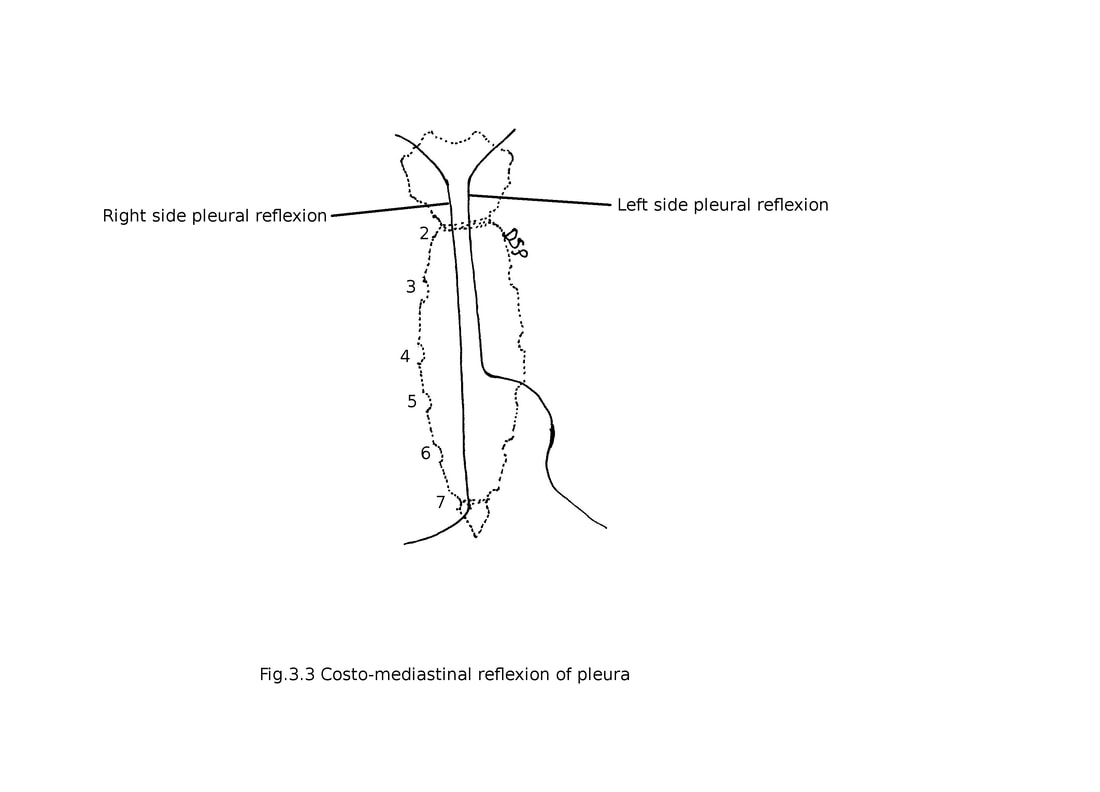
1) Costal : It covers inner surface of sternum, ribs, transversus thoracis muscle, intercostal muscles and vertebral bodies. Line of reflexion anteriorly goes downward and medially from sternoclavicular joint to sternal angle then downwards up to xiphisternal joint going laterally follows 7th costal cartilage and costodiaphragmatic line of pleural reflexion on right side. While on left side goes downward and medially from sternoclavicular joint to sternal angle then downwards up to 4th costal cartilage deviates laterally up to 6th costal cartilage and costodiaphragmatic line of pleural reflexion. Superiorly it is continue with cervical pleura at inner margin of first rib. Inferiorly continue with diaphragmatic pleura.
2) Diaphragmatic : It covers upper surface of the diaphragm. Laterally continue with costal pleura. Medially continue with mediastinal pleura.
3) Cervical : It is continuation of costal pleura above from medial border of first rib. It covers apex of the lung. It extends 3 - 4 cm above first costal cartilage. It is covered by suprapleural membrane. Suprapleural membrane is a musculo-fascial expansion showing attachment on inner margin of first rib and behind shows attachment on tip of transverse process of 7th cervical vertebra. This membrane is strengthened by scalenus minimus.
4) Mediastinal : It is forming lateral boundary of mediastinum. It shows reflexion over lung root and continue as pulmonary pleura. On right side it comes in relation with right brachiocephalic vein, superior vena cava, arch of azygos vein, brachiocephalic trunk, right phrenic nerve, right vagus nerve, trachea and oesophagus. On left side it comes in relation with arch of aorta, left common carotid, left subclavian, superior intercostal veins, left phrenic, left vagus nerves, recurrent laryngeal nerves, oesophagus, thoracis duct and left brachiocephalic vein.
Recesses :
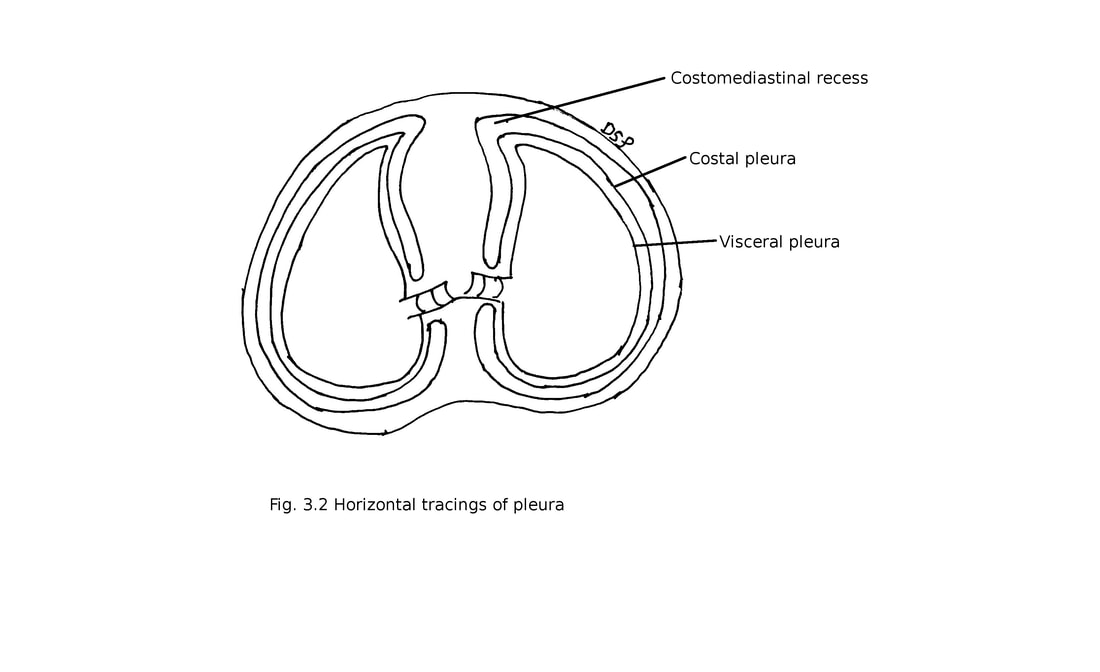
Pleura goes downwards to cover upper surface of lung. It forms costodiaphragmatic recesses below between costal and diaphragmatic pleura. Costomediastinal recesses forms anteriorly in relation with sternum and costal cartilage between costal and mediastinal pleura. Recesses provide space for expansion of lung.
Pleura is a serous membrane covered by mesothelium. There are two pleural sacs right and left covering respective lungs.
It shows two layers 1. Visceral or pulmonary 2. Parietal. These two layers are continuous with each other near hilum of lung. It forms a space between two layers known as pleural cavity.
1. Visceral or pulmonary pleura :
It covers surface of lung firmly attached to it. At hilum and pulmonary ligaments it continue as parietal pleura. It goes around the root of lung downwards as a fold of pulmonary ligament.
2. Parietal pleura : It shows attachment on inner surface of sternum, ribs, intercostal spaces, costal cartilages, diaphragm and vertebra. It shows four parts : 1) costal 2) diaphragmatic 3) cervical 4) mediastinal
1) Costal : It covers inner surface of sternum, ribs, transversus thoracis muscle, intercostal muscles and vertebral bodies. Line of reflexion anteriorly goes downward and medially from sternoclavicular joint to sternal angle then downwards up to xiphisternal joint going laterally follows 7th costal cartilage and costodiaphragmatic line of pleural reflexion on right side. While on left side goes downward and medially from sternoclavicular joint to sternal angle then downwards up to 4th costal cartilage deviates laterally up to 6th costal cartilage and costodiaphragmatic line of pleural reflexion. Superiorly it is continue with cervical pleura at inner margin of first rib. Inferiorly continue with diaphragmatic pleura.
2) Diaphragmatic : It covers upper surface of the diaphragm. Laterally continue with costal pleura. Medially continue with mediastinal pleura.
3) Cervical : It is continuation of costal pleura above from medial border of first rib. It covers apex of the lung. It extends 3 - 4 cm above first costal cartilage. It is covered by suprapleural membrane. Suprapleural membrane is a musculo-fascial expansion showing attachment on inner margin of first rib and behind shows attachment on tip of transverse process of 7th cervical vertebra. This membrane is strengthened by scalenus minimus.
4) Mediastinal : It is forming lateral boundary of mediastinum. It shows reflexion over lung root and continue as pulmonary pleura. On right side it comes in relation with right brachiocephalic vein, superior vena cava, arch of azygos vein, brachiocephalic trunk, right phrenic nerve, right vagus nerve, trachea and oesophagus. On left side it comes in relation with arch of aorta, left common carotid, left subclavian, superior intercostal veins, left phrenic, left vagus nerves, recurrent laryngeal nerves, oesophagus, thoracis duct and left brachiocephalic vein.
Recesses :
Pleura goes downwards to cover upper surface of lung. It forms costodiaphragmatic recesses below between costal and diaphragmatic pleura. Costomediastinal recesses forms anteriorly in relation with sternum and costal cartilage between costal and mediastinal pleura. Recesses provide space for expansion of lung.
Blood supply :
Parietal pleura supplied by intercostal, internal thoracic and musculophrenic arteries. Costal pleura supplied by intercostal and internal thoracic arteries branches. Mediastinal pleura supplied by bronchial, diaphragmatic, internal thoracic and mediastinal arteries. Cervical pleura supplied by subclavian artery. Diaphragmatic pleura supplied by arteries of diaphragm.
Visceral pleura supplied by branches of bronchial arteries.
From parietal pleura veins drains into azygos and thoracic veins. From visceral pleura veins drains into bronchial veins.
Lymphatic drainage : From parietal pleura lymph drains into intercostal, internal mammary, posterior mediastinal, diaphragmatic nodes and mediastinal nodes. From visceral pleura lymph drains into bronchopulmonary lymph nodes.
Nerve supply : Parietal pleura supplied by intercostal and phrenic nerves. Costal and peripheral part of diaphragmatic pleura supplied by intercostal nerves. Mediastinal pleura and central part of diaphragmatic pleura supplied by phrenic nerves. Pulmonary pleura supplied by sympathetic nerves from T4 and T5 segments.
Applied anatomy :
1. Pleuritis or pleurisy : Inflammation of pleura know as pleuritis. In pleural effusion pleuritis is present.
2. Pleural effusion causes collection of fluid in pleural cavity.
3. Paracentesis thorasis is a procedure for drainage of collected fluid in pleural cavity. For drainage needle is inserted in 6th intercostal space in mid-axillary line in relation to lower part of intercostal space.
4. Haemothorax : Collection of blood in pleural cavity.
5. Pneumothorx : Collection of air in pleural cavity.
6. Pyothrax : Collection of pus in pleural cavity.
7. Hydropneumothorax : Collection of both fluid and air in pleural cavity.
Parietal pleura supplied by intercostal, internal thoracic and musculophrenic arteries. Costal pleura supplied by intercostal and internal thoracic arteries branches. Mediastinal pleura supplied by bronchial, diaphragmatic, internal thoracic and mediastinal arteries. Cervical pleura supplied by subclavian artery. Diaphragmatic pleura supplied by arteries of diaphragm.
Visceral pleura supplied by branches of bronchial arteries.
From parietal pleura veins drains into azygos and thoracic veins. From visceral pleura veins drains into bronchial veins.
Lymphatic drainage : From parietal pleura lymph drains into intercostal, internal mammary, posterior mediastinal, diaphragmatic nodes and mediastinal nodes. From visceral pleura lymph drains into bronchopulmonary lymph nodes.
Nerve supply : Parietal pleura supplied by intercostal and phrenic nerves. Costal and peripheral part of diaphragmatic pleura supplied by intercostal nerves. Mediastinal pleura and central part of diaphragmatic pleura supplied by phrenic nerves. Pulmonary pleura supplied by sympathetic nerves from T4 and T5 segments.
Applied anatomy :
1. Pleuritis or pleurisy : Inflammation of pleura know as pleuritis. In pleural effusion pleuritis is present.
2. Pleural effusion causes collection of fluid in pleural cavity.
3. Paracentesis thorasis is a procedure for drainage of collected fluid in pleural cavity. For drainage needle is inserted in 6th intercostal space in mid-axillary line in relation to lower part of intercostal space.
4. Haemothorax : Collection of blood in pleural cavity.
5. Pneumothorx : Collection of air in pleural cavity.
6. Pyothrax : Collection of pus in pleural cavity.
7. Hydropneumothorax : Collection of both fluid and air in pleural cavity.